www.thetinman.org Copyright © All rights reserved.

Disclaimer: The material presented in this site is intended for public educational purposes only. The author is not offering medical or legal advice. Accuracy of information is attempted but not guaranteed. Before undertaking any diet, or health improvement program, you should consult your physician. The author is in no way liable or responsible for any bodily harm, physical, mental or emotional state of any patient reacting to any of the content on this site. Thetinman.org has not examined, reviewed or tested any product or service mentioned herein. We are not being paid to advertise or promote any product or service mentioned herein. The links are offered strictly as examples of resources available. The site assumes no responsibility or liability of any kind related to the content of external sites or the usage of any product or service referenced. Links to external sites were live at the time of creation of the link. Thetinman.org does not create content for or manage external sites. The information can be changed or removed by the external site’s administrators at any time and they are responsible for the veracity of their information. Links are provided to support our data and supply additional resources. Please report broken links to administrator@thetinman.org. Thetinman.org is not a charitable foundation. It neither accepts nor distributes donations or funds of any kind.

Classic stiff-person syndrome is found in the majority of cases presented. The diagnosis is clinical, based on symptoms after ruling out other neuromuscular differentials. Motor and sensory exams are normal.
w Symptoms typically present in the third to sixth decades of life
w Patients often have co-existing autoimmune diseases such as diabetes, autoimmune thyroid disease, vitiligo, pernicious anemia, epilepsy, and myasthenia gravis.
w Onset is rarely acute or sudden. There is a slow, gradual onset of aching and fluctuating stiffness and rigidity in the neck, abdominal, and/or upper and lower paraspinal muscles which can spread to proximal (close to the body) leg muscles and/or arms.
This extreme degree and pattern of stiffness and rigidity are highly suggestive of SPS.
w There can be considerable symmetrical pain.
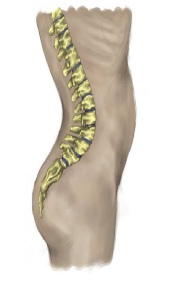
w Over time, rigidity of the paraspinal muscles can result in a fixed deformity of the spine and hyperlordosis (exaggerated curvature) of the lower spine. Paraspinal muscles can become grossly hypertrophied.
w As rigidity of the chest and abdominal muscles progresses, it can result in hunched shoulders and curvature of the upper spine (kyphosis). Stiffness of chest wall muscles can restrict respiration and lead to exercise intolerance. Esophageal dysmotility and swallowing difficulties contribute additional risk of aspiration. Abdominal spasms can cause early satiety.
w Rigidity of the trunk can become fixed, making it difficult to bend or turn at the waist. As postural reflexes are overridden by stiffness and flexibility is lost, gait becomes slow and awkward. Rigidity makes it difficult for a patient to “catch himself” when he falls. There is a high risk of injury from falls.
w Calf and foot muscles are rarely involved in classic SPS. However, foot spasm with dystonic posture has been reported. Prolonged lack of mobility may lead to stiffness in the hip, knee, and ankle joints.
w Superimposed spasms last minutes to hours and are easily visualized. The affected muscles become rock-hard and board-like. Palpation may provoke intense spasm. Spasms can become strong enough to fracture bone and rupture muscle.
The absence of these spasms in an untreated patient should raise doubts about the diagnosis of stiff-person syndrome.
w Patients exhibit heightened sensitivity to stimuli such as noise, touch, and emotional distress, which can set off painful muscle spasms and cause falls.
w Head retraction reflex and/or truncal retropulsion are sometimes present and elicited by tapping the nasal ridge, upper lip, chin, or between the eyebrows.
w Patients exhibit a fear of falling while ambulating in public or across uneven surfaces and in negotiating stairs, but not true agoraphobia.
w Seizures and concurrent epilepsy have been reported in a small percent of patients.
w Cranial muscle involvement is possible.
w Abnormal gaze and eye movements are possible.
w Paroxysmal autonomic dysfunction (including transient fever, sweating, fast breathing and heart rate, pupillary dilatation, and arterial hypertension) has been described.
w Depression due to loss of quality of life is seen in over half of the patients. The anxiety and fear response can be mistakenly viewed as psychosomatic illness. Due to the level of medications required to treat the spasms, patients are sometimes mislabeled as drug-seeking or malingering.
w Untreated or under-treated patients are at a high risk of suicide. Sudden withdrawal of treatment causes a rapid escalation of symptoms which can be life threatening.
w Patients are advised to carry a medical alert card stating this risk at all times.

The current criteria for a diagnosis was developed by Dr. Marinos Dalakas and refined and expanded by Dr. Lorisch et al.)
1. Prodrome of stiffness and rigidity in axial muscles.
2. Slow progression of stiffness resulting in impairment of ambulation.
3. Fixed deformity of the spine in general and pronounced lordosis.
4. Presence of superimposed episodic spasms precipitated by sudden movement, noise, or emotional upset.
5. Normal findings on motor and sensory nerve examinations.
6. Continuous motor-unit activity on electromyelogram abolished by intravenous diazepam.
7. Normal intellect.
8. Presence of either anti-glutamic acid decarboxylase antibodies (60% of patients) or anti-amphiphysin antibodies (<5%).

Stiff-Person Syndrome
Special Care & Handling Required
CLASSIC STIFF-PERSON SYNDROME